Comparative Analysis of Emergency vs. Outpatient Admissions in a Cardiovascular Unit
For this project, I analyzed a dataset containing two years of hospital admissions and discharge records from the Hero DMC Heart Institute. The project focused on a comparative analysis of emergency vs. outpatient admissions in the cardiovascular unit, with an emphasis on patient profiles, outcomes, and recommendations for improving care delivery and resource planning.
Dataset Overview
The dataset included 56 variables covering:
- patient demographics,
- admission type,
- length of stay (hospital and ICU),
- laboratory results,
- comorbidities,
- admission and discharge dates,
- and outcomes (discharged, discharge against medical advice, or expired).
Overview
Cardiology units often face challenges in efficiently triaging patients, particularly when distinguishing between emergency and outpatient admissions. Outcomes such as mortality, length of stay, and ICU use are influenced by comorbidity burden, abnormal lab results, and acuity at admission. This project explored how admission type impacts patient trajectory and how these insights can guide resource allocation, triage practices, and risk evaluation.
Methodology
The analysis was performed using Pandas for data cleaning and manipulation, and Matplotlib for visualization.
To see the raw code, visit my Github page.
Data preparation steps included:
- Removing duplicate entries to ensure dataset integrity.
- Standardizing date formats and calculating discharge dates using admission date and duration of stay.
- Validating calculated lengths of stay against reported values.
- Checking for duplicates, missing values, and inconsistent entries. Null values were retained in laboratory results, since imputation could misrepresent patient conditions.
- Categorizing key laboratory results as normal or abnormal based on clinical reference ranges.
- Counting the number of comorbidities per patient.
- Renaming and standardizing selected columns while removing redundant ones for clarity.
Key Findings
-
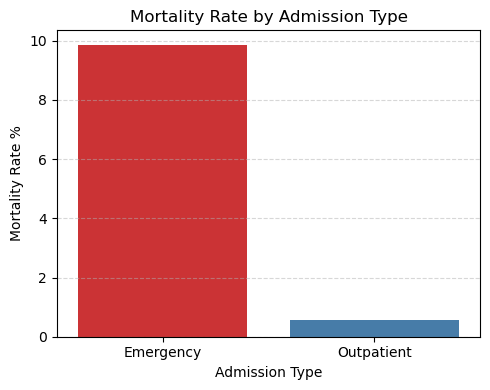
Mortality Rate:
- Emergency admissions had a mortality rate of 9.86%, compared with only 0.58% for outpatients.
- This highlights the acute and life-threatening nature of emergency cases, underscoring the need for earlier identification of high-risk patients.
-
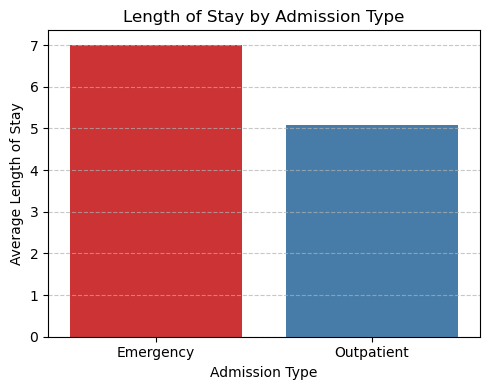
Length of Stay:
- Emergency patients stayed an average of 7 days, compared to 5 days for outpatients.
- Longer stays reflect both higher severity and potential delays, which increase capacity pressures and costs.
-
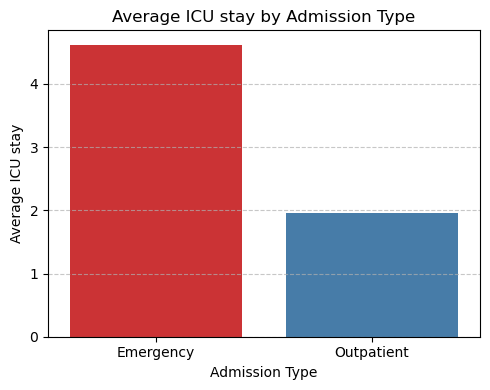
ICU Utilization:
- Emergency patients required longer and more variable ICU stays (4.62 days vs. 1.96 days for outpatients).
- Extended ICU stays contribute to capacity issues and care delays, emphasizing the need for predictive tools at intake.
-
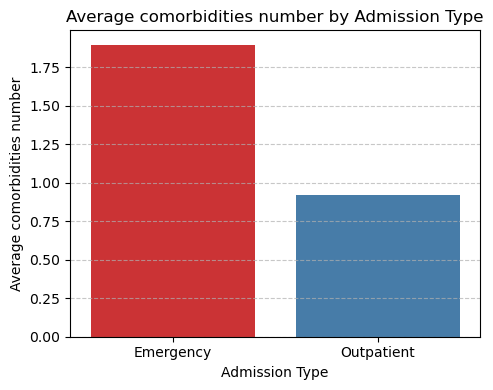
Comorbidity Burden:
- Emergency patients presented with an average of 1.89 comorbidities, while outpatients averaged 0.92.
- This nearly twofold difference reflects the higher complexity of emergency cases and the greater strain they place on ICU resources.
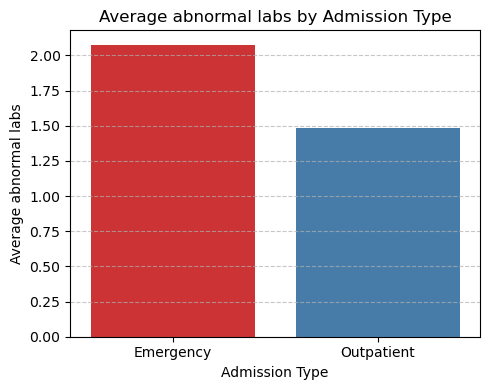
- Abnormal Laboratory Results:
- Emergency patients averaged 2.07 abnormal results, compared with 1.48 for outpatients.
- A higher frequency of abnormal values indicates greater clinical instability and the need for rapid intervention.
Recommendations
Based on these findings, several strategies were proposed:
- Early Risk Assessment: Rapid identification of high-risk patients at admission using early warning systems, comorbidity scoring, and lab result screening.
- Streamlined Emergency Care: Implementation of standardized pathways and accelerated diagnostic protocols to reduce delays and optimize bed usage.
- ICU Resource Optimization: Predictive evaluation of ICU needs at intake to balance resources and minimize capacity bottlenecks.
- Hospital Capacity Management: Proactive discharge planning and monitoring of ICU occupancy to improve efficiency.
- Data-Driven Planning: Leveraging historical data to forecast future resource demands and improve long-term strategic planning.
Conclusion
The analysis revealed clear distinctions between emergency and outpatient cardiovascular admissions in terms of mortality, length of stay, ICU requirements, comorbidity burden, and laboratory results. These findings underscore the importance of data-driven strategies to improve patient outcomes, allocate resources effectively, and reduce systemic strain.
It is important to note that the results and recommendations are based solely on the provided dataset and may not capture the full complexity of real-world clinical environments. Nevertheless, the project demonstrates how analytical approaches can provide actionable insights for hospital management and patient care optimization.